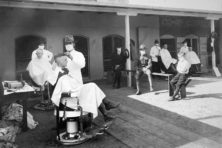
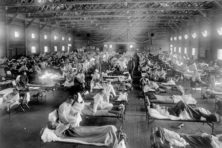
Lessons from the 1918 Spanish Flu
- Share
- Tweet
- Pin
- Share
The first book I wrote, more than four decades ago, was a history of the then-132-year-old Ritenour School District, where my husband and I both worked for many years.
As the coronavirus pandemic began to make the news in the U.S. early in March, I remembered writing in that book about similar conditions when the Spanish flu reached St. Louis more than a century earlier. I recalled how differently St. Louis, then the sixth-largest city in the country; and Philadelphia, the third-largest, responded to the crisis and how tragically those differences affected the death toll in each city. It prompted me to refresh my memory of what I’d written about that time in Ritenour’s history and to research what went on nationally in 1918-19.
The Ritenour District, which had begun in a one-room log cabin in 1846, offered its first high school classes in the fall of 1914. Ten freshmen – eight girls and two boys – enrolled. Two years later, enrollment had jumped to 29. Four girls from the original freshman class graduated on May 17, 1918.
Four months later, the influenza epidemic had begun to sweep across the U.S., and Ritenour schools were closed indefinitely. Classes resumed late in November, but they were closed again a few days later when the superintendent reported 73 elementary pupils absent, a teacher ill at home and another in the hospital. Students missed nearly three months of school, and the only member of the 1919 senior class died before graduating.
Nearly a billion people fell ill worldwide, and 50 million died, including an estimated 675,000 in the United States. Those hit hardest were healthy people ages 20 to 40.
Meanwhile, America was in the waning months of World War I, and city officials across the country were under pressure to sell war bonds, or “Liberty Loans.” Many communities had scheduled huge parades to welcome returning soldiers and promote patriotism and bond sales.
The first case of flu among civilians in Philadelphia was reported on Sept. 17, 1918, but authorities downplayed its significance and continued to allow large public gatherings.
Philadelphia’s parade was scheduled for Sept. 28. City officials, led by Health Commissioner Wilmer Krusen – a political appointee with no prior public-health experience – ignored doctors’ pleas to cancel it, even though 118 city residents, as well as 600 sailors and 47 civilians at the Philadelphia Naval Yard, were ill with the flu, and some had already died.
In advance of the parade, the city distributed 20,000 flyers urging citizens to cover their mouths when they coughed or sneezed. Ten times that many people watched the two-mile-long event. Three days later, according to TheWeek.com, every bed in Philadelphia’s 31 hospitals was occupied. School closures, bans on public gatherings and other social-distancing interventions were not implemented until Oct. 3.
But it was too late. By then, 45,000 citizens were already infected, and by mid-November, 12,000 Philadelphians were dead. The city morgue was capable of holding only 36 bodies, so corpses piled up on sidewalks. Within six months, half a million city residents had become ill, and the death toll totaled 16,000.
By the time the pandemic reached the Midwest, St. Louis had had time to prepare. The first cases in the city were reported on Oct. 5. Although Philadelphia had taken 16 days to respond with interventions, St. Louis took just two. That 14 days’ difference, experts believe, represented three to five “doubling times” for the epidemic – a tragedy for Philadelphia that St. Louis avoided.
Dr. Max Starkloff, the St. Louis health commissioner for most of the years between 1895 and 1935, marched into the office of Mayor Henry Kiel on the day when the first cases of flu were diagnosed and said, “We’re shutting the city down.” Kiel is reported to have responded, “Over my dead body!”
But Starkloff prevailed, and on Oct. 7, strict measures to promote social distancing went into effect. Schools, movie theaters, saloons, sporting events, churches and other public gathering spots were ordered to close.
As the flu continued to rage in November, Starkloff imposed an even stricter quarantine, closing down all businesses except for banks, newspapers, embalmers and coffin makers. Ambulances waited at Union Station to take any passengers who appeared to be ill directly to a hospital. Police officers and mail carriers wore masks as they made their daily rounds. Inside factories that couldn’t shut down during wartime production, doctors roamed the floors to watch workers for any signs of flu symptoms.
The quarantine was lifted temporarily on Nov. 18, but it was reinstated when the flu roared back in December. By Dec. 10, the flu peaked in the city, with 60 deaths in one day. After that, there was a sharp decline in reported illnesses, and the quarantine ended just after Christmas. Even with Starkloff’s far-sighted actions, the flu killed nearly 3,000 St. Louisans during the last three months of 1918.
But thanks to those actions, the death rate in St. Louis was the lowest among the 10 biggest cities at the time. Philadelphia’s was eight times greater.
In Milwaukee, then the 13th-largest city in America, Health Commissioner Dr. George Ruhland acted aggressively to close schools, saloons and other public places the moment the flu struck, plastering the city with ads warning people to stay home.
Even after restrictions were lifted, dance-hall revelers on New Year’s Eve wore six-layer gauze masks. A story in the Journal-Sentinel described them as looking like a “band of holdup men from the neck up.” The death rate in Milwaukee – 0.6 percent – was the lowest of any large city in the country.
San Francisco was not so fortunate. Residents celebrated on Nov. 21, 1918, when a whistle blast signaled that their masks could come off. A story in the Chronicle reported “sidewalks and runnels [gutters] strewn with the relics of a torturous month.”
In January, when the third wave of the flu arrived, business and theater owners fought back against reinstating restrictions on public gatherings, arguing that masks would provide sufficient protection, as had been the case earlier.
It didn’t work. San Francisco ended up with some of the highest influenza death rates in the country. A scientific analysis in 2007 concluded that had the city kept all of its anti-flu protections in place through the spring of 1919, the number of deaths could have been reduced by 90 percent.
The last century saw almost complete eradication of polio, mumps, measles and rubella, but as for progress in preparedness for another pandemic? Not much.
Three years ago, Michael Osterholm, one of the top biosecurity and infectious-disease specialists in the world and head of the Center for Infectious Disease Research and Policy at the University of Minnesota, predicted a global flu pandemic that would rival the 1918 flu. In his best-selling book, Deadliest Enemy, published in 2017, he predicted what such a pandemic would look like if it emerged in China. During an interview in March, he said, “It’s exactly what happened.”
*********************
The Spanish Flu Probably Didn’t Start in Spain
Spain was one of only a few major European countries to remain neutral during World War I. Unlike in the Allied and Central Powers nations, where wartime censors suppressed news of the flu to avoid affecting morale, the Spanish media outlets were free to report on it in gory detail.
News of the sickness first made headlines in Madrid in late May 1918, and coverage increased after King Alfonso XIII came down with a nasty case a week later. Because nations undergoing a media blackout could read in-depth accounts only from Spanish news sources, they naturally assumed that the country was the pandemic’s ground zero.
Then Where Did It Start?
The exact source of the Spanish flu is unclear, but it’s thought to have taken root in early March 1918 among World War I soldiers at Camp Funston, part of the U.S. Army base in Fort Riley, Kansas.
Several thousand soldiers there were treated for a mysterious flu that killed 38. Soon tens of thousands of soldiers who had trained in Kansas were off to the battlefields of France, Belgium and Italy. Within six to eight months, the flu had exploded across Europe, Africa and the United States.